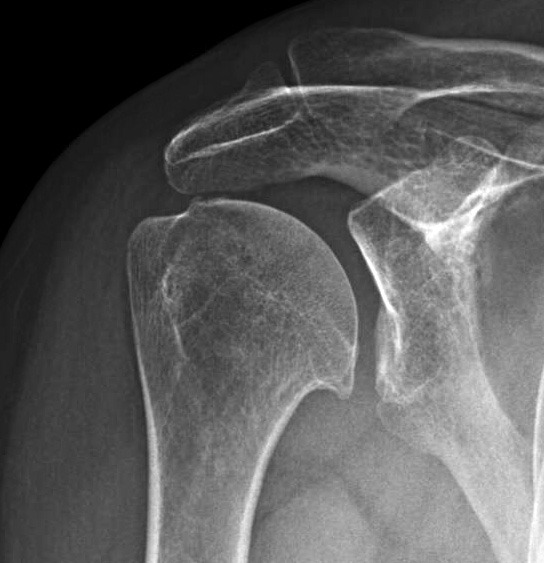
- Why does glenohumeral arthritis cause deep shoulder pain even without heavy activity?
Glenohumeral arthritis affects the main ball-and-socket joint of the shoulder. As the smooth cartilage lining wears down, movement becomes less fluid, and the underlying bone is exposed. This leads to joint inflammation, causing pain even during simple activities. Many patients notice discomfort at rest, at night, or when lying on the affected side.
Unlike muscle pain, arthritic pain often feels deep within the joint and is associated with stiffness. The shoulder may ache after periods of inactivity and loosen slightly with gentle movement. Over time, joint changes such as bone spurs can further restrict motion and contribute to pain. This explains why symptoms may persist even without strenuous use. Early assessment helps distinguish arthritis from other causes of shoulder pain and allows timely management to reduce discomfort and preserve movement.
- How is glenohumeral arthritis different from normal age-related shoulder stiffness?
While mild stiffness can occur with age, glenohumeral arthritis involves structural damage to the joint. Progressive cartilage damage, narrowing of the joint gap, and bone changes contribute to shoulder pain, limited range of motion, and reduced daily function. This is different from age-related stiffness, which usually improves with activity and does not cause persistent pain.
Patients with arthritis often notice grinding, catching, or reduced range of motion when lifting the arm or rotating it. Tasks such as dressing, reaching overhead, or fastening garments become difficult. These symptoms tend to progress over time rather than fluctuate. Recognising this distinction is important, as arthritis responds better to targeted treatment than to simple stretching or rest alone.
- Can physiotherapy really help when the joint cartilage is already worn?
Physiotherapy does not restore lost cartilage, but it plays a vital role in managing symptoms. Strengthening the muscles around the shoulder improves joint support and reduces stress on damaged surfaces. Improved movement patterns also help reduce inflammation and pain.
Rehabilitation focuses on maintaining shoulder flexibility, enhancing posture, and strengthening the rotator cuff and shoulder blade–supporting muscles.
Many patients experience meaningful improvements in pain and function with consistent physiotherapy, particularly in early- to moderate-stage arthritis. Even when surgery is considered later, good muscle conditioning improves outcomes. Physiotherapy is therefore a cornerstone of non-surgical management.
- What role do injections play in managing glenohumeral arthritis?
Injection therapy is commonly used to manage pain and inflammation when other non-surgical treatments are not effective. Corticosteroid injections can provide short- to medium-term relief by calming joint inflammation. Other options, such as lubricating injections, may improve movement and comfort in selected cases.
Injections cannot cure arthritis, but they can help control pain, improve comfort, and delay the need for surgery. Their effects vary between individuals and are usually temporary. Injections are best used as part of a broader treatment plan that includes physiotherapy and activity modification, rather than as a standalone solution.
- When should surgery be considered for glenohumeral arthritis?
Surgery is considered when pain and stiffness significantly interfere with daily life despite appropriate non-surgical treatment. Difficulty sleeping due to pain, loss of independence in daily tasks, and reduced shoulder function are common reasons for discussion.
The type of surgery depends on age, activity level, and the condition of surrounding structures. Modern shoulder replacement options aim to reliably relieve pain and restore function. Surgery is not rushed and is carefully timed to match symptom severity and patient goals. A thorough discussion ensures realistic expectations and informed decision-making.
- What can I expect long-term if I manage glenohumeral arthritis without surgery?
Many people manage shoulder arthritis successfully for years without surgery. Symptoms often progress slowly, and with appropriate care, pain can be controlled and function maintained. Activity modification, regular exercise, and periodic medical review are key.
However, arthritis is a degenerative condition, and symptoms may gradually worsen. Regular follow-up helps reassess treatment options and ensures timely intervention if needed. Early attention to symptom changes helps avoid sudden loss of function and preserves shoulder health.
- Does glenohumeral arthritis affect sleep?
Yes. Shoulder arthritis commonly causes night pain, especially when lying on the affected side. Inflammation within the joint and reduced cushioning lead to discomfort at rest. Adjusting sleeping position, using supportive pillows, and appropriate treatment can significantly improve sleep quality.
- Can shoulder arthritis cause weakness even if muscles are intact?
Yes. Pain and joint stiffness can limit movement, leading to reduced muscle use over time. This results in functional weakness even when the muscles themselves are healthy. Targeted physiotherapy helps maintain strength and coordination.
- Is glenohumeral arthritis always progressive?
The condition is degenerative, but progression varies. Some people experience slow changes with long periods of stability. Early management, activity modification, and strengthening can slow symptom progression and maintain function for many years.
- Can weather changes make shoulder arthritis pain worse?
Some people notice their shoulder pain flares during colder or damp weather. While weather does not cause arthritis, changes in temperature and air pressure can increase joint sensitivity and stiffness. Keeping the shoulder warm, staying gently active, and maintaining regular exercise often helps reduce these temporary flare-ups.