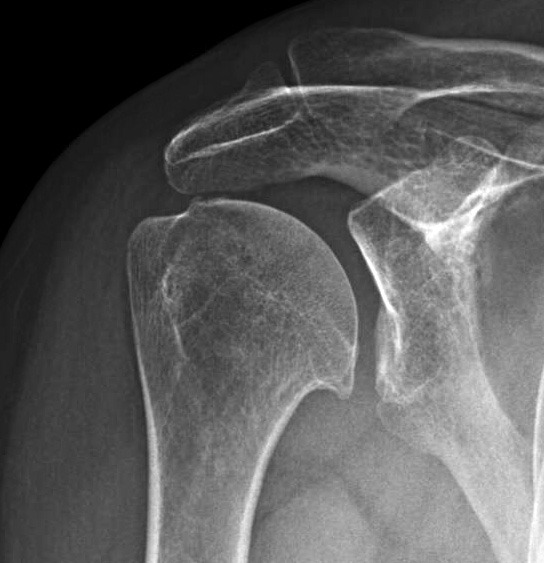
- What are the signs and symptoms of glenohumeral arthritis?
The most common symptom of glenohumeral arthritis is pain due to rubbing of bones within the shoulder joint.
The pain increases with time, gradually over years. It is commonly present at night, and interferes with sleep. The other common symptom is loss of motion because of chronic inflammation, pain and disuse of the shoulder joint, fractures or previous surgeries. There may be weakness of supporting muscles. Disuse may cause wasting away of shoulder muscles. Swelling and tenderness may also be present. You may hear crepitus (clicking or crunching sound) during movement of the shoulder joint.
- How is glenohumeral arthritis diagnosed?
The doctor will ask your medical history and discuss symptoms. Most patients report an increase in pain over years. The doctor will ask if you have any other conditions like previous trauma or surgery to the shoulder, an infection in the shoulder, previous rotator cuff injury or rheumatoid arthritis in other joints. The doctor will do a physical examination of the shoulder to check if other deformities exist. The doctor may ask to go for imaging techniques like X-ray, CT scan, MRI of the shoulder to confirm a diagnosis of glenohumeral arthritis. X-ray will show irregularity of the joint surface, osteophytes and bone erosion.
- How is glenohumeral arthritis treated?
The treatment of glenohumeral arthritis depends on the severity. Mild glenohumeral arthritis is often treated by rest, NSAIDS (non-steroidal anti-inflammatory medicines) – such as ibuprofen or naproxen, exercises to increase range of motion and strength whereas mild to moderate glenohumeral arthritis pain is controlled by corticosteroid injections (cortisone shots) for cases that do not respond to NSAIDS.
Glucosamine and chondroitin are also helpful as they aid in cartilage formation. Viscosupplementation therapy cushions the joint surfaces. Hyaluronic acid is injected directly into the joint to improve joint lubrication and reduce friction during movement. If glenohumeral arthritis is severe, operative treatment is recommended. Debridement surgery and Shoulder Arthroplasty (replacement of shoulder joint).
- What are the complications that occur after surgery?
The potential complications that occur after surgery are bleeding, nerve injury and infection. Nowadays perioperative antibiotics and intraoperative antibiotics are given which have reduced chances of infection.If infection is chronic, that is present for more than 6-12 weeks, it requires the removal of the implant.
Blood loss is another common complication during shoulder replacement surgery and you may require transfusion.
Nerve injury can also occur during shoulder replacement surgery but they are usually temporary. Normal functioning returns over time.
Component failure also occurs and is more common with the glenoid component of a total shoulder arthroplasty.
- How much time does it take to recover?
Recovery may vary patient to patient.
The patient, physician, and physical therapist requires to work together in order to have good and fast results.
During the first 6-8 weeks after surgery, the shoulder is immobilized with a sling or a cast.
A passive range of motion exercises should be performed to prevent stiffness as it maintains functional motion in the shoulder.
After 6-8 weeks, when soft tissues are healed, an active range of motion can start.
Afterwards, a strengthening program begins, focusing on the rotator cuff muscles and those that strengthen the scapula.
A maintenance program of shoulder exercises for whole life is recommended.Complete recovery usually takes 4-6 months.