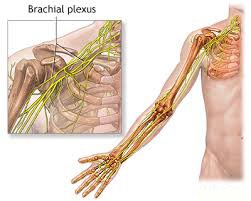
Brachial plexus injury can happen in many ways, including:
CONTACT SPORTS – Many soccer players experience symptoms like stingers and burners. It happens when the brachial plexus nerves get stretched beyond their limit during collision with other players.
DIFFICULT BIRTH – Newborns can suffer from brachial plexus injuries. High birth weight, breech presentation or prolonged labour can account for this. If the baby’s shoulders get wedged within the birth canal, there is an increased incidence of brachial nerve palsy. Generally the upper nerves are damaged.
TRAUMA – Number of trauma, including motor vehicle and motor cycle accidents, falls or bullet wounds can lead to brachial plexus injury.
TUMOURS AND CANCER TRATEMENTS – Tumours can grow in the area of brachial plexus. Moreover, they can put pressure on the brachial plexus. Apart from that, when the chest area undergoes radiation treatment there is a chance of brachial plexus damage.
With time many brachial plexus injuries in both adults and children heal without any lasting damage. Having said that, all brachial plexus injuries should not be taken lightly as some may cause temporary or permanent problems such as:
STIFF JOINTS – Joints can stiffen due to paralysis of the hand or arm. This can make movement very difficult though you may eventually regain full range of motion. Because of this, your physician may recommend physiotherapy during your recovery phase.
PAIN – Pain arises out of nerve damage and it can be chronic.
NUMBNESS – If you feel your hand or arm numb, you may burn or injure yourself without even realising it.
MUSCLE ATROPHY – Nerve regeneration takes time. In some cases it can take even years to heal completely. During that time the affected muscle may degenerate due to lack of use.
PERMANENT DISABILITY –Your recovery from a brachial plexus injury depends on a number of factors, including your age, location, severity of injury. In rare cases even with surgery people ends up with permanent muscle weakness or paralysis.