The past decade has witnessed the rise in popularity for biological treatment options when it comes to cartilage repair. The reason for these therapies gaining prominence possibly has to do with minimal invasiveness, improved healing time, and faster recovery. These methods of repair also have the added advantage of being rich in growth factors or stem cells that will aid the recovery and regeneration process better.
These therapies also happen to be a less expensive alternative to surgical procedures. Some examples of biological therapies for cartilage repair can include platelet-rich plasma, bone marrow aspirate concentrate, and cell-based therapies. These methods have found to be especially beneficial in conditions like focal chondral lesions and early osteoarthritis where it is so crucial to get treatment early.
Bone marrow that is replete with a number of bone growth factors as well as stem cells is greatly utilized for a number of orthopedic procedures. Bone marrow is also quite often aspirated to make use of the growth factors and cells for tissue repair applications including bone remodeling. In orthopedics, bone marrow aspirate is also used in the preparation of allograft bone for implantation.
The many advances in medical technology have made the process of harvesting bone marrow and utilizing it intraoperatively much easier nowadays. Bone marrow can be harvested from areas like iliac crest, vertebral body, calcaneus, proximal or distal tibia, distal femur, and proximal humerus.
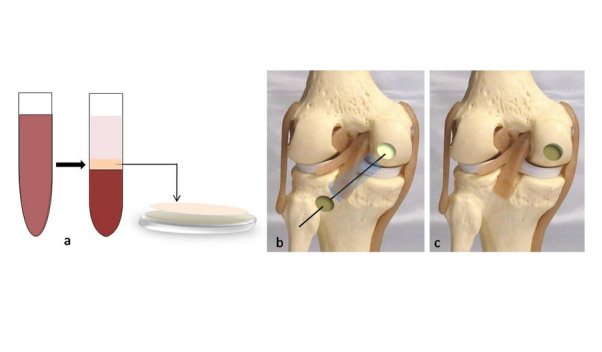
Once the aspirated bone marrow is analyzed, it then goes through a process to create a bone marrow aspirate concentrate. This concentrate is then injected into the body in areas of degeneration or injury to promote healing. A process of centrifugation helps to isolate cells that contain growth factors.
Popular bone marrow aspirate techniques include the likes of Mosaicplasty or autologous osteochondral autograft/allograft transfer system or OATS used to treat both focal chondral defects as well as cases of osteochondritis dissecans. Mosaicplasty is a reconstructive bone grafting procedure that can be performed entirely arthroscopically, as a combined arthroscopic and mini-arthrotomy procedure, or as an open technique. This is ideal for patients between the age 15 to 50 years and with a body mass index less than 30.
Mosaicplasty involves the removal of small osteochondral cylinders from low weight bearing surfaces of the affected joint or another joint in the same individual and transplanting them in a mosaic-like formation into focal chondral or osteochondral defects in the affected joint. Both open and arthroscopic mosaicplasty require a short rehabilitation period and normal daily activity can be resumed after 5 to 8 weeks. But this is again largely dependent on the individual lesion and other patient factors. When mosaicplasty is combined with ligament reconstruction or osteotomy, brace use is required.
The osteochondral autograft transfer system (OATS) is a procedure employed for medium sized areas of discrete damage whereas mosaicplasty is employed for even larger but discrete areas of damage. This procedure is similar to mosaicplasty though, it involves the use of a larger, single plug that usually fills an entire defect like in the case of ACL tears.
For enquiries and online appointments, send a message to www.BangaloreShoulderInstitute.com/contact
For informative videos related to Shoulder problems and their treatment options, Sports Injuries and other orthopedic conditions, visit the YouTube channel Bangalore Shoulder Institute – https://www.youtube.com/channel/UCJldz_Osg88qFYM99IEsjew
