- By shoulderadm
- In Blog
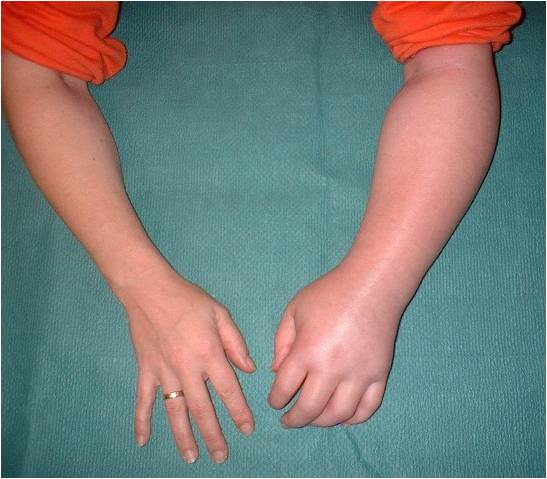
Shoulder-Hand Syndrome
Shoulder-Hand syndrome is a relatively common occurrence after stroke. Usually, the person has a stroke that leaves them paralyzed on one side. Recovery of the paralysis is subjective, varies between patients. Often the lower extremities recover quicker than the upper ones. For reasons unknown, some people are left with significant weakness in the hands that can be quite painful. When the pain is quite severe in the hand and the shoulder on the paralyzed side the condition is called shoulder-hand syndrome.
Symptoms:
• Shoulder Pain
• Hand Pain
• Numbness
• Elbow Pain
• Wrist Pain
• Tingling
• Burning
• Stiffness
• Swelling
• Discoloration of the hand
Description:
There are two types of shoulder-hand syndrome.
- Type 1 occurs post an injury or illness that did not directly damage a nerve in the affected area
- Type 2 happens after a distinct nerve injury
Though the triggers may vary, both types of shoulder-hand syndrome have the same symptoms and go through the same three stages of disease, which are:
Stage I: Acute
This stage may last upto three months and begins with rapid onset of widespread swelling, joint stiffness and tenderness at the top of the hands. The affected person can feel a burning pain and sensitivity to touch. Hand can become pale due to narrowing of the blood vessels in the hand. On moving the hand, substantial pain in the shoulder and hand can be felt. The pain is more constant and longer lasting. There can be increased warmth and redness in the hand. There may be faster-than-normal nail and hair growth and excessive sweating. Patchy areas of bone loss can be seen on x-rays of the hands.
Stage II: Dystrophic
This stage can last upto 3 to 12 months. Swelling is more constant and skin wrinkles disappear. Skin temperature cools off. Fingernails can become brittle and the pain is broad-based. Stiffness increases and the affected area becomes extremely sensitive to touch.
Stage 3: Atrophic
This stage occurs after one year. It is characterized by absence of swelling, tenderness and pain, but hand movements are limited because the fingers may be stiff or clawlike, resembling Dupuytren’s contractures. A significant loss in the density of the bones can be seen on x-rays taken at this stage.
Causes:
Injuries such as falling on the hand, breaking the wrist bone, heart attack, stroke, and possibly use of certain drugs (such as barbiturates) can lead to this condition. However, the precise way that shoulder-hand syndrome develops is unknown. One theory is that a “short circuit” in the nervous system is responsible. This “short circuit” causes overactivity of the sympathetic (unconscious) nervous system which affects blood flow and sweat glands in the affected area.
Symptoms generally appear after injury or surgery. Other causes include pressure on a nerve, infection, cancer, neck problems, stroke, or heart attack. Some people seem to be genetically predisposed to develop this disorder than others.
Doctor examination:
After discussing your past medical history and symptoms, the doctor will do a close examination of the affected hand. People with shoulder-hand syndrome are unusually protective of the involved limb. Even a light touch may evoke expressions of severe pain.
Tests:
There is no single test that can make the diagnosis of shoulder-hand syndrome. Some imaging studies, such as x-rays, bone scans, and magnetic resonance imaging (MRI) scans can help your doctor to arrive at a firm diagnosis.
Treatment:
For a meaningful recovery of this condition, treatment should be started as early as possible. This may prevent the disease worsening further. Treatment usually includes a combination of therapies such as:
Non-surgical treatments:
Medications: Non-steroidal anti-inflammatory drugs (NSAIDs), oral corticosteroids, anti-depressants, blood pressure medications, anti-convulsants and opioid analgesics are medications recommended to relieve symptoms.
Injection therapy: Injecting an anesthetic near the affected sympathetic nerves can reduce symptoms. This is usually recommended early in the course of shoulder-hand syndrome in order to arrest further progression to the later stages.
Biofeedback: Increased body awareness and relaxation techniques may help with pain relief.
Therapy: Active exercise that stresses on normal use of the affected limb is indispensable for permanent relief of this condition. Physical and/or occupational therapy are important in helping patients regain normal use of the affected hand. Medications and other treatment modalities can bring down the intensity of the pain, thus allowing the patient to engage in active exercise.
Surgical treatments:
If non-surgical treatments do not bring the desired result, there are surgical procedures that may help to deal with the syndrome in a better way.
Spinal cord stimulator: Tiny electrodes are implanted along your spine and deliver mild electric impulses to the affected nerves.
Pain pump implantation: A small device that delivers pain medication to the spinal cord is implanted near the abdomen.
Psychological evaluation and counseling is another significant treatment modality for shoulder-hand syndrome.
For questions related to Shoulder Hand Syndrome, send a message to www.BangaloreShoulderInstitute.com/contact
Q and As – Shoulder Hand Syndrome
1.What is the shoulder hand syndrome?
The term shoulder hand syndrome is used to describe painful disabilities of the upper limb due to disturbances of the sympathetic nerve supply to the affected limb. The various symptoms experienced due to shoulder hand syndrome are a result of reflex stimulation of the sympathetic nervous system. Any or all such disabilities have a common or similar underlying mechanism that involves the blood vessels and nerves.
2. What causes shoulder hand syndrome?
The shoulder hand syndrome is most commonly seen in association with conditions like a heart attack (or myocardial infarction), some kind of trauma, and stroke (or hemiplegia). Infrequently, it has also been observed after a herpes zoster infection, gonococcal arthritis, diffuse vasculitis, cervical osteoarthritis, and thrombophlebitis.
It is caused due to any disturbance or trauma to the tissue which affects the sympathetic nervous system, associated with the spinal cord, which provides the nerve supply to the upper limb and the shoulder. The elbow is rarely involved in shoulder hand syndrome.
3. What are the ways in which shoulder hand syndrome can be prevented after a stroke?
After a patient has suffered a cardiac or cerebral stroke, it is likely for them to develop shoulder hand syndrome. There are protocols in place that are used to prevent shoulder hand syndrome from developing in patients who are in the early stages of their recovery from a stroke. These mainly involve different types of passive shoulder and hand movements that can be performed by the patient alone or with the help of a physical therapist. Active movements can also be done by the patient if it is not painful. It helps reduce hand edema and stiffness.
4. What are the symptoms associated with shoulder hand syndrome?
The shoulder hand syndrome is also called Steinbrocker syndrome. The symptoms seen with shoulder hand syndrome, which may last from weeks to years, are:
- Painful shoulder with a disability to move and limited range of motion.
- Swelling and color changes in the overlying skin.
- Pain and stiffness of the hand and fingers.
- Change in color may vary from deep red to cyanotic blue or pale.
- In the early stage, the hand is warm due to elevated temperature.
- Loss of fat from the affected limb.
- Osteoporosis of the bones of the hands, tendon tightness and pain, deformities of the fingers.
The symptoms seen in a particular case of shoulder hand syndrome can range from a mild form to prolonged progressive syndrome.
5.How is shoulder hand syndrome treated?
The shoulder hand syndrome is diagnosed based on clinical presentation. Three-phase bone scintigraphy is believed to be the most useful additional diagnostic test.
The treatment for shoulder-hand syndrome initially consists of conservative treatment options like physical therapy. Another option is the administration of corticosteroids. One should consider the role of proper physical therapy in improving the results of other treatments as well as in preventing the syndrome. Many stroke patients may have contraindications to corticosteroid therapy, hence other methods of effective treatment are crucial.





