- By shoulderadm
- In Blog
Arthroscopic Decompression of Paralabral Cysts in Shoulder Surgery
Paralabral cysts are fluid-filled sacs that can form around the labrum of the shoulder joint. While some cysts cause no symptoms and may be discovered incidentally, others can lead to persistent pain, weakness, restricted movement, or even nerve compression. When non-surgical treatments fail to provide relief, arthroscopic decompression offers a minimally invasive and effective surgical option to restore shoulder function.
Understanding Paralabral Cysts
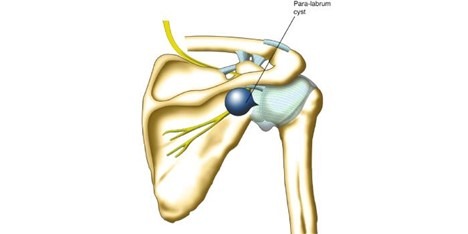
The labrum is a ring of cartilage that deepens the shoulder socket (glenoid), helping to stabilise the joint. Paralabral cysts typically develop when joint fluid escapes through a tear or defect in the labrum and collects in nearby tissues. These cysts are most frequently located near the superior or posterior aspects of the labrum.
In some cases, the cysts compress nearby structures, particularly the suprascapular nerve, leading to weakness in the shoulder muscles responsible for lifting and rotating the arm. Patients often report a dull, persistent ache in the shoulder, limited mobility, and sensations like clicking or catching when moving the joint. Nerve compression can further result in muscle atrophy and functional impairment if left untreated.
Indications for Surgical Intervention
Not all paralabral cysts require surgery. Many asymptomatic cysts can be monitored or managed conservatively with rest, physiotherapy, and anti-inflammatory medications. However, surgery may be recommended when patients experience ongoing pain, functional limitations, or symptoms of nerve involvement that fail to improve with conservative treatment.
The Arthroscopic Decompression Procedure
Arthroscopic decompression is carried out by inserting a thin camera and specialised tools through small keyhole incisions around the shoulder joint. This allows the surgeon to clearly visualise the internal structures of the joint while minimising soft tissue disruption.
During the procedure, the cyst is identified and drained, allowing the trapped fluid to escape and relieving pressure on surrounding tissues. In most cases, the underlying labral tear responsible for the cyst formation is also repaired during the same operation to prevent recurrence. Surgeons may use additional techniques, such as injecting dye into the cyst beforehand, to aid in precise localisation and complete decompression.
Expected Results After Surgery
Arthroscopic decompression with labral repair has shown excellent outcomes, reducing pain, restoring shoulder movement, and improving muscle strength. In cases of nerve compression, shoulder muscle weakness often improves as healing progresses. The minimally invasive approach also allows for smaller incisions, quicker recovery, and fewer complications. Recurrence of cysts is uncommon when the labral tear is fully addressed.
Recovery and Rehabilitation
After the procedure, patients generally use a sling for a few weeks to safeguard the repaired area during initial healing. Physiotherapy is then introduced to gently improve shoulder movement, rebuild strength, and restore overall function. Most people are able to resume their usual activities, including sports, within three to six months, depending on the complexity of the cyst and the degree of labral repair performed.
Conclusion
Arthroscopic decompression of paralabral cysts provides a safe, effective, and minimally invasive solution for ortho patients experiencing persistent shoulder pain or nerve-related symptoms. By addressing both the cyst and any associated labral damage, this modern surgical approach offers long-lasting relief and allows most patients to regain full shoulder function and return to an active and healthy lifestyle.
For enquiries and online appointments, send a message to www.BangaloreShoulderInstitute.com/contact
For informative videos related to Shoulder problems and their treatment options, Sports Injuries and other orthopedic conditions, visit the YouTube channel Bangalore Shoulder Institute – https://www.youtube.com/@BangaloreShoulderInstitute





